What Can I Control as a Physician during COVID?
Sometimes the most amazing lessons happen at the most unexpected times.
Yesterday I did a ‘wellbeing hackathon’ with my daughter. Since she’s twelve, I thought I’d be teaching her a lot of what I knew about innovation and well-being. Instead, I did a lot of learning myself.
She and I have been building an internet-of-things connected device, thanks to an innovation award from the Brigham Health Physicians Organization. Our device was designed to be as simple as possible, measuring one thing: “are you happy or stressed?”. It is an early detection system for the epidemic of physician burnout - a ‘happy button’ to measure stress among healthcare workers.
And then the pandemic began in earnest…
As the COVID-19 pandemic has continued to grow, we’ve begun to see how important resiliency is to effective healthcare functioning. Care systems are being rapidly redesigned. While our happy button is fun and an interesting design challenge, we see a new urgency to capturing stress signals from healthcare staff during this crisis. Stress across healthcare organizations has been high for a long time, but this pandemic will take it to extremes. The happy button project aims to capture a longitudinal, real-time view of worsening stress across organizations, that may signal overall declining resilience in our healthcare system.
We expect stress to rise during a pandemic, obviously, but we also want to know the rate of rise (is it a cliff?), whether it’s affecting everyone equally or specific groups disproportionately, and understand better the correlation between happiness and stress. We also want to know whether hospital interventions that try to address staff stress make any difference (we all recall those times when someone tried to make us less stressed, but made it worse). All of these stressors have direct costs to our healthcare workers, to the health system and to our society as a whole.
So my daughter and I talked about expanding our project with other tools for measuring stress among health care workers. We pondered a smartphone app, smartwatch app, texting bot, and voice skill. I was all ready to start developing one of these with her until she so wisely said, “But Dad, aren’t there already apps that let you do this?” and pointed me to a review article she had read about ‘great apps you’ve never heard of’. Yup, there’s an app for that.
So our hackathon pivoted. Instead of hacking together a new product, we designed a way to systematically evaluate and study existing ‘stress apps’ and their risks and benefits.
My daughter chose to start with an app featuring a little A.I. penguin “that makes you feel heard”. As we explored the app, the little penguin offered what seemed to be an offhand image, but which struck me as really profound - a small image of the circles of control. In the diagram, the inner circle is what you can control, the outer circle what you cannot control.
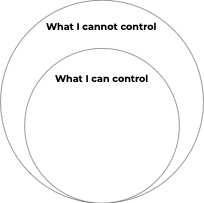
Today as I worked in the stressed-out environment of the hospital trying to prepare my patients, the facility, and myself for the surge ahead, I found it really helpful to think about these circles of control. As a physician, it feels like there are some grey areas between these circles: if only I knew more, if only I was a better advocate against X, if only my patient listened to me, if only I communicated more clearly.
I sat down and drew my own version, trying to capture what could I control during COVID-19:

In making this diagram, I realized that for a physician, there are more than two circles: in addition to the things that I can and cannot control, there are areas where my actions can matter, where I can influence but not control the outcome. These are areas where I deeply wish I could control the outcome; I wish I could stop my patients or my family from becoming sick, or from dying. But at the time I write this, we don’t yet have a cure or a vaccine for COVID-19, and so the best I can do is try to take every action available to me. To try and influence the best possible outcome, and give the best care possible.
My daughter and I continue to work on that stress-signal system so that we might begin to rebuild resiliency in American healthcare, but for now: remember the circles, and find, nourish and act from your strengths - that which you can control.
Here is a blank chart for you to use to create your own map.
References:
- A delightful another example of a control chart from TheCounselingTeacher.com is here
- http://www.skilledatlife.com/things-we-cannot-control-or-change-in-life/
